Some Women Say…
that the loss of their hair is more devastating than their cancer diagnosis. You may feel like your hair is essential to looking and feeling like yourself.
Hair loss is also a visible sign of illness and can impact self-image and self-esteem. You may feel vulnerable and anxious.
You’re not alone… support is here, every step of the way.
Prior to Hair Loss
- Depending on your specific treatment protocol, your hair could thin or fall out completely during treatment.
- Your oncology team will be able to inform you when to expect hair loss.
- If you want a wig to match your current hairstyle, colour and texture, consider looking for a wig before starting treatment.
- You can also take pictures of your current hair from all sides and bring those with you when choosing a wig.
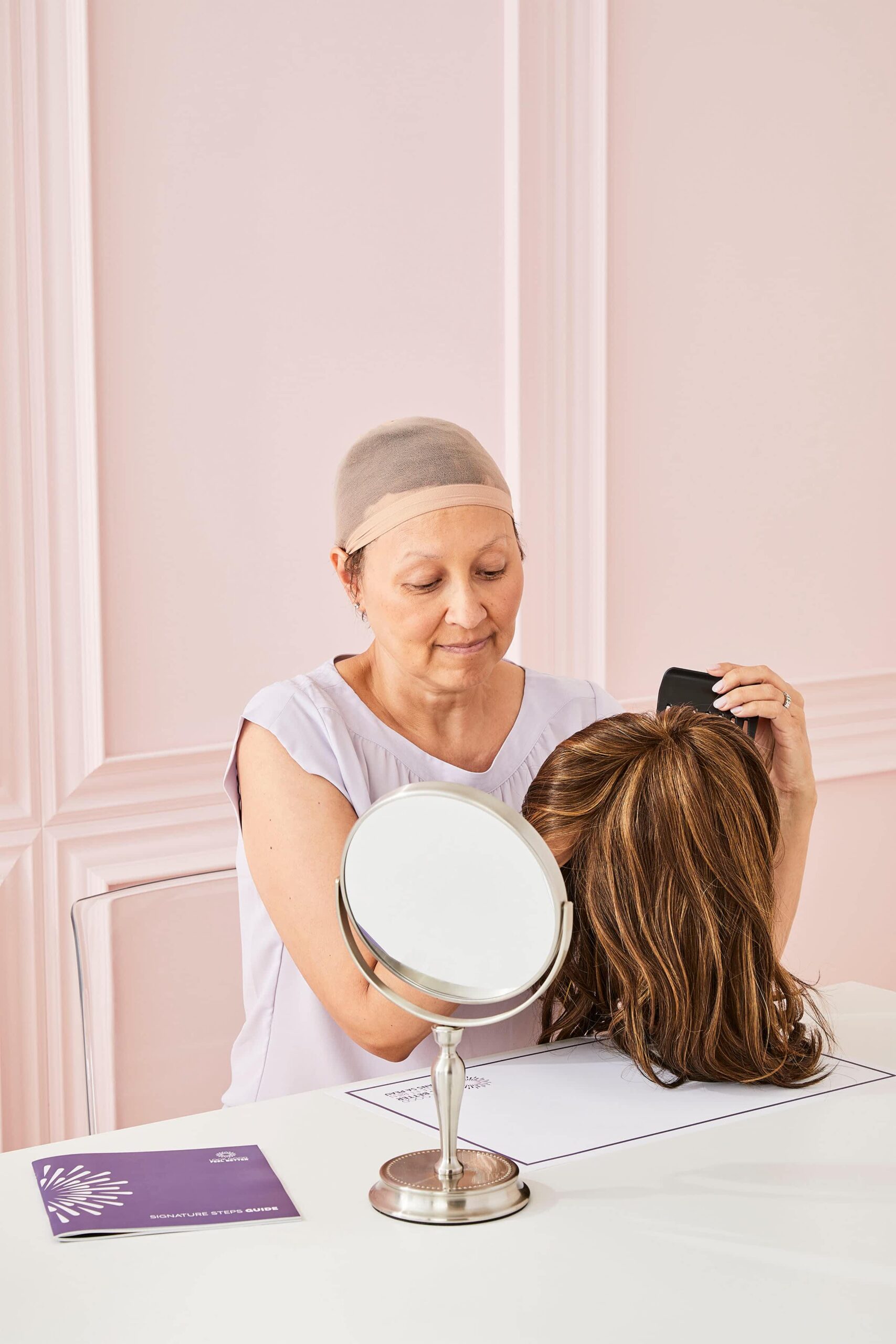
Shaving your head
- Watching hair fall out in clumps can be emotionally distressing. Some people prefer to shave it off before too much hair falls out.
- A very short haircut (e.g. 1/8 of an inch) can help ease scalp sensitivity and ease the emotional distress of seeing hair fall out in clumps.

Thinning Hair
If you notice that your hair is thinning, consider these things:
Don’t colour your hair right now. It may break and make it thin more quickly.
As the texture of your hair may change and become brittle, using a a hydrating shampoo and conditioner will help your hair feel softer.
Consider cutting your hair shorter than you usually wear it. It can help your hair look thicker and make hair loss less noticeable. Also, short hair doesn’t put stress on already weak hair follicles.
If possible, avoid overusing blow dryers, curling irons, hot rollers, hair sprays and any products with an alcohol base.
When sleeping, use a satin-like pillowcase to minimize tugging your hair at the scalp.
Full Hair Loss
- When hair loss starts, your scalp will be very sensitive, and hair will fall out gradually
- This is when you might want to cut your hair to at least 1/8 of an inch
- You also may want to wear a sleep cap during the day and at night to catch your hair
- Consider having two sleep caps – one for day, the other for sleeping

Caring for your Scalp
- When you’ve lost your hair, your scalp may become drier
- Gently massage your scalp with your facial moisturizer to make it feel more comfortable and increase circulation to your stressed hair follicles
- Caring for your scalp will greatly reduce sensitivity and itchiness, allowing you to wear a wig, scarf, or hat more comfortably

Let’s navigate this together
Join a community that understands. Receive expert advice, useful resources, and compassionate tips throughout your cancer journey in the LGFB newsletter
Newsletter Form
Easy Skincare Tips During Cancer Treatment
Taking care of your skin while going through cancer treatment might sound like a lot, but keeping it simple can really help. A gentle skincare routine can make your skin feel better and help with some of the side effects, like dryness or irritation.
Here’s a step-by-step routine that’s easy to follow, even on tough days. With the right products and a soft touch, you’ll be giving your skin the love it needs.
A healthy skin care regiment before and during cancer treatment gives you the best chance of lessening the severity of side effects on your skin.
Product Info: Moisturizers (from light to rich)
Not all moisturizers are the same. Here’s the breakdown — start light and go richer if your skin needs more hydration:
Gels – super light, barely-there moisture
Lotions – light but a bit more hydrating
Creams – great for normal to dry skin
Balms – thicker, perfect for dry or flaky skin
Ointments – super rich, heavy-duty moisture
Not everything has to change during treatment.
Get tips about nails, skincare makeup and hair in our Teens Workshop.
Let’s navigate this together
Join a community that understands. Receive expert advice, useful resources, and compassionate tips throughout your cancer journey in the LGFB newsletter
Newsletter Form
Tips to keep your hands and feet healthy:

-
Avoid cutting your cuticles. Instead, use cuticle cream to help combat dryness, splitting and hangnails.
-
Moisturize with a rich hand cream.
-
Keep nails short.
-
Wear rubber gloves while doing chores as excessive exposure to water can lead to fungal infection of the nail bed.
Nail Polish and Nail Salons
If you’d like to use polish, soft, neutral shades of pink will lend a healthy- looking finish
Use an oily acetone-free polish remover. Acetone is very drying and can make nail problem worse during treatment
When visiting a salon, make sure the staff has worked with clients undergoing cancer treatment (or at least knows how to take extra precautions to keep you safe and healthy)
Let’s navigate this together
Join a community that understands. Receive expert advice, useful resources, and compassionate tips throughout your cancer journey in the LGFB newsletter
Newsletter Form
Working as an oncology nurse has been my dream for so long. Losing my mom to breast cancer definitely influenced my decision to work in oncology and my desire to help people. It’s incredibly rewarding. But one thing’s for sure – I never expected to be on the other side of the diagnosis, facing cancer myself.
I especially didn’t expect it at just 30 years old – and 24 weeks pregnant with my first child. My mom passed away when I was only two years old, and to suddenly get the same diagnosis while I was on the verge of becoming a mom myself was beyond terrifying. I practically blacked out when I heard the news. I kept thinking, “What? I’m pregnant. This isn’t supposed to happen.” It was quite the curveball, to say the least.
While it was the most difficult news to receive, I’m so grateful they caught it early. I’m thankful that there were chemo medications I could take that were safe for my unborn son. I have the most phenomenal doctors and nurses – my colleagues in the cancer centre in Sudbury, Ontario, became my caregivers overnight. I have a wonderful support team through my husband, Ryan, and my step-mom, who I really think of as my mom, as she’s been a mother to me my whole life. She has been my rock. And this whole ordeal has given me a completely new perspective on facing cancer, despite the fact that I’ve cared for cancer patients for seven years now.
For example, although I supported cancer patients in their journeys everyday as a nurse, I underestimated the mental and emotional toll that cancer treatment would have on me. For one, losing my hair was so tough. I had always been like, “Oh, it’s just hair, it’ll grow back.” But it’s not just hair. It was part of me and my self-esteem and how I presented myself to the world.
I already knew about Look Good Feel Better (LGFB) through my work in the chemo room, and it became such a valuable resource for me. I signed up for a workshop right away, and boy, was it ever awesome. As a nurse, I had often heard about the impact of LGFB but experiencing it firsthand was completely different. Like losing my hair, I didn’t fully grasp how much it would mean to me until I was living it.
I took my mom to the workshop as my support person, and it was so good for the soul. I learned some great hair and makeup tips, but more than that, it gave me a powerful sense of hope. It helped me reclaim my self-esteem and made the scary experience I was going through feel a whole lot less scary. I loved connecting with other women who were going through what I was going through. Having cancer can feel so lonely – I had all the support in the world, but people didn’t really understand what I was going through, because, well, they didn’t have the diagnosis. Being able to share my experience with the women in the workshop was really special.
I’m so grateful that LGFB exists, and that my future patients will have the opportunity to attend the workshops. And now, I can speak to the experience personally. When I’m able to go back to work, I know I’ll be able to connect with and support my patients on a whole new level.
My son, Matthew, has arrived, and things feel so much better now. A lot of the anxiety and fear of the unknown that I experienced – about cancer, about being a first-time mom – have faded. This journey has given me a deeper understanding of resilience, both for myself and my patients.
I thought I had moved on. I thought that my cancer journey was behind me — far in the past. When a routine mammogram led to a new breast cancer diagnosis in 2023, it was a complete shock. My cancer had recurred after 13 years.
At first, I beat myself up over the diagnosis. I thought I had been doing everything right — eating well, working out, taking care of myself. “What did I do wrong?” I wondered. “How could this have happened?” I started to doubt my every move, every bite that I put in my mouth. My self-confidence declined. But I quickly realized that blaming myself wasn’t going to help. I had to act. I needed to take back control.
This time, I chose a double mastectomy with reconstruction. It felt like the safest option — I didn’t want to rely on mammograms anymore. And although I was reluctant to undergo chemo again after my painful first experience, I knew it was necessary. Thankfully, the treatment was a little easier this time. I received a new scalp cooling treatment that helped prevent hair loss, which made a huge difference for me emotionally. Though the chemo still brought its challenges — nausea, fatigue, and rashes — keeping some of my hair helped me feel like I hadn’t completely lost myself to the disease. Scalp cooling was a new innovation that hadn’t been available to me the first time around, so I was grateful for the opportunity to try it out.
Building a support system was also a priority for me. I’m from Mauritius, a tropical island off the coast of South Africa, and most of my family is still there, so I had to create my own network here. I discovered Look Good Feel Better (LGFB), and attending their workshop made a huge difference. My “look” is very important for me, and it was comforting to feel pampered and cared for, especially after all the blows and bad news I’d been receiving. The workshop helped me to regain confidence and connected me to a group of women who understood exactly what I was going through.
I also started a walking group for cancer patients and later joined a dragon boat group for breast cancer survivors. Looking at the strength of these paddlers made me feel strong, too. If they can do it, so can I. It was encouraging. After my first cancer experience, I was eager to move on and forget about it. But now, I realize there’s power in staying connected with the cancer community and with other survivors. I’m a two-time survivor. This is my life and my reality, and I accept it now.
This time, my son also played a bigger role in my recovery. He was just a toddler the first time I had cancer, but now, as a teenager, he became part of my support system. He loves photography, and whenever I did my makeup, he’d take photos of me and edit them. It made me feel good about myself and it became our bonding time, and those photos now hold a special place in my heart.
Today, I cherish every moment with my husband and son. We cook, go for walks, shop, watch movies — those little everyday moments mean everything to me now. I’m grateful for each day and, rather than cry about what happened to me or worry about the future, I choose to live in the present. Cancer may be part of my story, but it doesn’t define who I am.
By JC Chessell
It’s funny – as I sit here about to blog on my ‘expertise’ with hats and scarves, I find myself wearing a knitted toque aptly placed on my head. I do not know which came first: my love affair with hats or the loss of hair, which led me to my love affair of hats. Whichever it is, I still find myself wearing hats and head coverings A LOT. And I love it!
Today, I wear them out of personal freedom and choice but wearing hats during my treatment is forever a memory etched on my heart. Having cancer made it less of an option and more of a necessity for me to wear hats, but I enjoyed the look and the way they warmly protected my head.
I’d like to share my personal guide to “Covering Your Head During Cancer Treatment”.
Let’s say you’ve just been diagnosed and are thinking of covering your head with SOMETHING. You will discover there are various options for your head covering: hats, scarves and wigs (natural and synthetic).
Having so many choices gives us each more control as we move through our personal journeys. You will find that having a head covering, such as a scarf or hat, gives such a nice, quick pick-me-up and you may feel better about yourself and your outward appearance.
I mainly wore hats through my chemotherapy and radiation sessions. I kept my natural-hair wig for special occasions, like weddings and events.
Since I was diagnosed at the end of summer going into fall and cold winter weather followed, practically speaking, hats were my favourite and most sensible option. As you decide which head covering to go with, try to think about what look you want to present.
Hats give us SO many options, from fun and sassy to a more laid-back, practical type of look. You will see how your face changes as you wear different shapes, from the wide-rimmed to the smaller fisherman cap. And it only takes a second to put on a hat. Again, the choice is yours.
Scarves, I find, are a better option for spring/summer weather. Your scalp has breathing space due to the softer fabrics and overall, scarves have a lighter feel on the head. If you allow your imagination to run really wild, you can create a gorgeous scarf ‘up-do’ with layers of different scarves, thus allowing for height and dimension to frame your face—think Eryka Badu.
If you are deciding on a scarf option, my only advice would be to stay away from silk since the fabric slides off easily on bald or short hair scalp and will become more of an annoyance rather than anything else. The rest is up to you. And this is really where you get to play up different looks
Thankfully, new companies pop up offering us so many options with fabrics, colours and texture. And here’s a little do-it yourself tidbit: go to Fabricland, pick out a pattern that catches your eye—one that speaks to you. Ask the sales associate to cut off a specific amount of it (enough to wrap around your head at least twice) and make into a headscarf yourself. You may need to practice the wrapping a few times but soon enough, you’ll be an expert.
You should know that Look Good Feel Better workshops offer head/scarf wrapping info catering specifically to you and me, so that we can become more comfortable with how to wear our scarves in different ways. There are also lots of scarf-tying tutorials on YouTube, to give you even more ideas. You can start with this from Look Good Feel Better.

I was a new translator for Look Good Feel Better when I was offered the chance to attend a workshop to see for myself how a session was run.
I had already translated a number of testimonials from people who’d experienced a workshop, and what always stood out was the warm welcome from the volunteers, their expertise and their respect for the participants. Some mentioned how, once the workshop had begun, apprehensions disappeared and were replaced by joy—a feeling not always present during cancer. Others said that being surrounded by people going through the same experience as them gave them much-needed moral support, without realising it. For others still, the workshop was energising, as it broke the social isolation caused by the almost daily medical appointments, the omnipresent fear during the ordeal, the gruelling treatments, and the exhaustion that overtook them as time went by.
The testimonials echoed the scale of the challenges a person needs to overcome during cancer. However, when I attended a workshop, I was able to see another side of the story: the volunteers, like fairies, were busy preparing the room with care and rigour. Sure moves, no doubt performed a thousand times before, were carried out with enthusiasm and team spirit; we weren’t welcoming the Queen of England, but it just seemed the same! It was beautiful, it was real. Most of them had already done a full day’s work for their employer, but these specialists in make-up, skin care or hair prostheses had chosen to commit themselves to their community out of generosity and solidarity. The women who were about to come forward were in great need of the expertise of these volunteer specialists, and they understood this.
I took a seat at a table and, as soon as the first participants arrived, I saw the magic happen. The volunteers knew how to read the participants: the welcome was both friendly and respectful, never intrusive; everyone had their own space, depending on whether they were more reserved or more open.
These women who had come that evening to learn how to look ‘normal’ again, even though nothing in their lives was normal at the time, these women who had chosen to leave their homes in spite of great fatigue, unpredictable nausea or a morale that wasn’t always up to scratch, found themselves gathered in this room for (essentially) the same reasons: the desire to take back control of their lives, against all odds. They were going to discover make-up tips and tricks to redraw their lost eyebrows, to restore their complexion, to take care of their dull skin and their nails damaged by chemotherapy and radiotherapy. And perhaps they would be tempted to try on a wig to camouflage a now bald head, or a scarf that they’ll learn to wear in a variety of clever ways.
From that evening in February, I remember the spirit of sisterhood that springs naturally from a Look Good Feel Better workshop: women helping other women they don’t know, whom they may never see again. In time, some of them may forget the names of the others, these angels who were there for them for an evening; but the warmth of their exchanges will remain with them forever. As the American novelist and poet Maya Angelou put it so well: ‘People will forget what you said, they will forget what you did, but they will never forget how you made them feel’. For a few hours, the volunteers and participants will have been cosmic sisters, sisters of the heart. For a few hours, they will have shared a complicity and a friendship that normally takes years to develop between two people, through living side by side and sharing life experiences. That’s the power of a Look Good Feel Better workshop.
When I was offered the job of translating content for Look Good Feel Better, I hesitated at first. I felt uneasy. I wasn’t sure if I wanted to, or even if I could, write about such a difficult subject—women affected by a serious illness that often leads to harsh treatment. I’d had breast cancer a year earlier and, a few years later, would be overcoming a second one that would require even tougher treatments. I finally agreed, but gave myself the right to withdraw if the experience proved too harsh. Then I realised that this mission to look good and feel better was a regular (and happy) reminder that human nature is fundamentally good. In fact, during the second cancer, I only kept Look Good Feel Better as a client. I insisted on continuing this work, because the stories and testimonials had a calming effect on me. Look Good Feel Better reminded me every day that I wasn’t alone. And everything is so much sweeter when you don’t feel alone, isn’t it?
It was on Christmas morning — while in the shower, thinking of my children and the celebrations and everything that needed to be done — that I first felt the lump. I wanted to believe it was nothing, just like the doctors had told me before, when I’d had clogged milk ducts while breastfeeding — but deep down, I knew something was different this time.
When I left Bangladesh and came to Canada five years ago with just my husband and two small children, I never dreamed that I’d soon be facing stage 3 breast cancer in a new land, thousands of kilometres away from my family. I felt so very alone. And I had a hard time accepting my diagnosis. I’ve always lived a healthy, disciplined lifestyle. In my family, everyone looked to me as the example of good health — I was the one who knew what foods to eat and how to live the right way. I did everything right, and yet still, I was the one who got cancer. It didn’t seem fair.
I struggled to accept what was happening to me, but one thing was clear: I had no choice but to face whatever was coming. I have kids, I have a family — I wanted to live.
My treatment involved eight rounds of chemotherapy, a lumpectomy, and 19 rounds of radiation. I hid my pain, sickness, and sadness from my husband and son and daughter as much as possible. I didn’t want my husband to lose strength — he had so much on his shoulders, taking care of me and the kids. I had no one to turn to, no one to talk to. I was desperately stressed out and frustrated. And I felt so helpless — I’m a very independent person who suddenly wasn’t able to do much on my own.
Fortunately, I realized that this wasn’t a permanent situation. I knew I would be alright after my treatment, and so I accepted the pain and the reality of what I was facing. I endured the vomiting, nausea, and painful burns from radiation. And little by little, things started to look up. I found support. I found strength. And through the big dark cloud that is cancer, I found small rays of hope.
Every cloud has a silver lining, or as we say in Bangladesh, “shesh bhalo jar, shob bhalo tar” – “all’s well that ends well,” basically. Despite the hardships, cancer brought me unexpected gifts. When my hair grew back after my treatment, for the first time ever it was curly — something I had always wanted. Post-chemo, my skin is so much better. And I got to model again, thanks to Look Good Feel Better (LGFB). In my home country, I had a modelling career, but that all stopped when I came to Canada. Participating in the LGFB photo shoot brought back so many good memories. The feeling of being in the spotlight again was incredible.
Cancer has also made me a better person. I’m much stronger mentally now and I have a deeper sense of gratitude for life. I’m prepared to be a good advisor for anyone else going through a cancer journey. And I really want to contribute, to give back. I want to share my story and my positivity, and to support other cancer patients — especially back in my home country, where cancer treatment resources are limited. In Canada, I got the best cancer treatment possible. But Bangladesh is a developing country, and those who have cancer there are suffering immensely. One day, I hope to return to share what I’ve learned and support those who need it most.
When my doctor told me I needed to fast-track fertility treatments if I wanted to have more children in the future, I was overwhelmed with emotion. I was 33 and suddenly the option of having more children — the spontaneity, the joy of it — wasn’t mine anymore. I didn’t want to tell my partner, who didn’t have any children of his own yet. I felt like I was robbing him of an experience he might have naturally had with someone else, someone who wasn’t going through breast cancer. It made me feel flawed, as though something was wrong with me.
Eventually I did tell my partner, and he was very supportive. He accompanied me to my treatments. But opening up about my diagnosis was hard. In Caribbean culture, especially among the older generation, people tend to be very private about their health. When I found out I had cancer, I wanted to keep the news to myself — even from my partner, family, and friends. But as things progressed, I realized I couldn’t do it alone.
I’d had a lumpectomy years ago, for a benign lump, which I had kept secret. I thought I could do the same this time — have a bit of chemo and downtime and then go back to my regular life and work as a nurse, with no one the wiser. I didn’t want my mother to worry. “Here we go again,” I said to myself. “I can do this.” But this time was different. I didn’t realize how much my treatment would break me down physically. Suddenly, I couldn’t even walk to the bathroom or wash my face on my own. I told my family and they stepped in to help.
My sister was an absolute godsend. She moved in and helped with all the day-to-day stuff — laundry, groceries. But most importantly, she really helped with my 10-year-old daughter. She took her to the movies, did her nails, and took her to her dance lessons and recitals, making sure her life wouldn’t be completely turned upside down.
I had trouble breaking things down and explaining what was going on to my daughter. Kids learn about cancer at school through Terry Fox, so naturally she asked if I was going to die like he did. I couldn’t answer her questions without falling apart, so having my sister there — and also getting my daughter into a children’s support group — was essential.
My treatment — chemo, a mastectomy, radiation, and IV therapy — took everything from me physically, mentally, and emotionally. I felt like cancer had stripped me bare, leaving me with no say, no control, nothing.
And then I was introduced to Look Good Feel Better (LGFB). Honestly, I wasn’t going to go. I was feeling awful and I didn’t want to socialize. I was very closed off and isolated. But I put my fear aside and attended the workshop, and I’m so grateful I did. The air felt so loveable when I got there — so welcoming, inviting, uplifting, and warm. It ended up being the most amazing experience. Everyone was talking and joking around, being so supportive. I didn’t expect to feel beautiful when I walked out. LGFB is like a sisterhood. When I was feeling broken and bare, it lifted me up and helped me to feel loved.
Today, I’m getting used to a new normal. I’ve had to accept that I’m never going to feel the way I did before cancer. But I’ve also realized that it’s okay to lean on others and to find strength in sisterhood.
One question everyone may have as they begin their cancer treatment is ‘what are the side effects of my cancer treatment?’ The truth is, is that, while there are many common side effects from chemo, radiation, immunotherapy and drugs, your treatment experience will be different from anyone else. So, what’s ‘normal’? Your medical team may give you a booklet on what to expect, but the reality is, there is no ‘normal’.
Hair loss, fatigue, constipation, diarrhea, headache, nausea are all common side effects from cancer treatment. But you may also be dealing with loss of balance, strength and coordination. Others experience nerve tingling, “burning” or numbness. It’s also possible that you may not have any of these side effects. Your reaction to your treatment is as individual as your diagnosis itself.
In the past, a good patient was often described as someone who kept questions to a minimum, who followed all the advice that their healthcare professional provided, who didn’t complain or voice their concerns, and didn’t speak out about something they didn’t understand. Over the years, medical professionals have begun to realize that their patients are individuals, with minds of their own and ideas and questions about their own healthcare.
Enter, Dr. Margaret Fitch, a professor at the University of Toronto with a background in nursing and expertise in oncology and the psychosocial and emotional side of cancer. Dr. Fitch identifies the difference between ‘person-centered’ and ‘patient centered’ care. Your care is a partnership. Doctors, nurses and social workers bring knowledge and expertise, but you are the expert on you and your personal experience. Person-centered care calls on medical professionals to listen, work in partnership with you and to better understand what your life is like and to pay close attention to how any suggestions made may impact you.
Dr. Fitch offers some important take aways to help you in your efforts to ensure your care is ‘person-centered’.
Embrace Your Right to Ask Questions: It’s crucial to remember that you have the right to ask questions about your care and treatment. Even if it’s difficult to speak up, your health and well-being are paramount. Take time at home to write down your questions when you’re relaxed, and bring them to your appointments. Don’t hesitate to be firm and confident in asking for the information you need.
Utilize All Available Resources: While your time with your physician is limited, don’t hesitate to ask a nurse or another healthcare professional for additional support. Healthcare teams often work together, and they can help ensure that your concerns are addressed. It’s okay to use multiple strategies to get the information and support you need.
Understand That “Normal” Doesn’t Mean “Okay”: If you’re told that certain side effects or feelings are normal, it’s important to recognize that this doesn’t mean you have to accept them without support. There is help available, and you don’t have to navigate these challenges alone. Speak up about what you’re experiencing and ask about the resources and services that can provide relief.
Recognize the Uniqueness of Your Experience: Cancer is not just one disease, but many, each with its own treatments and side effects. What you go through may be completely different from someone else’s experience, even if the diagnosis sounds similar. Don’t feel pressured to compare your journey to others; instead, focus on what you need and seek out the right support for your specific situation.
Explore Your Options: The treatment and support options available to you are diverse. Whether it’s joining a group, seeking one-on-one counseling, or trying different therapies, it’s essential to find what works best for you. Don’t be afraid to explore different approaches until you find the one that feels right.
Stay Informed About New Treatments: Medical advancements, like targeted therapies, are constantly evolving. These treatments can be more precise and may reduce some of the more challenging side effects associated with traditional chemotherapy. Keep the conversation open with your healthcare team about new options that may be available to you.
Value Your Individuality: Remember, your journey is uniquely yours. While it’s helpful to hear others’ experiences, what works for someone else may not be the best fit for you. Trust in your instincts, ask for the information you need, and choose the path that feels most supportive to your individual needs and circumstances.
In Episode 2 of “Facing Cancer Together,” you will hear from several women undergoing treatment, each with their own unique version of ‘normal.’ Additionally, Dr. Fitch delves into the concept of ‘person-centered care,’ offering deeper insights into this compassionate approach to treatment. Tune in for a compelling discussion that highlights the diverse experiences of these women, the importance of personalized care and how you can advocate for yourself during your own cancer journey.